AI-Powered Diagnosis: How CeaseMyPain Can Save Millions from Misdiagnosis and Medical Malpractice in India and Canada?
AI-powered tools like CeaseMyPain are redefining the frontlines of healthcare. With the power to analyze patient-reported symptoms, identify red flags, and support clinicians with structured insights, CeaseMyPain directly addresses the cognitive and system failures that drive most diagnostic errors — saving both lives and costs.
Every consultation across India — over 4 billion annually — represents an opportunity to prevent harm and empower patients with personalized, evidence-based guidance. In Canada, the same principles apply: roughly 3 consultations per person per year mean over 120 million diagnostic encounters, where AI can enhance quality and reduce avoidable harm. [1][2][3][4][5][6][7]
The Misdiagnosis Epidemic: India and Canada
India: Scale and Consequences
Misdiagnosis in India is an under-recognized epidemic. Studies estimate ~5.2 million medical-malpractice incidents annually, with up to 43.5 crore (435 million) diagnostic errors each year — stemming from high disease burden, low doctor-to-patient ratios, fragmented records, and limited time per visit. [3][6]
Such errors lead to:
- Delayed or incorrect treatment
- Avoidable hospitalizations and deaths
- High out-of-pocket expenditure (OOPE)
- Escalating legal action and mistrust
Canada: Different System, Similar Challenge
Canada, despite universal healthcare, faces similar diagnostic vulnerabilities:
- 5–15% of primary care encounters contain a diagnostic error.
- Delayed cancer and cardiac diagnoses remain among the top causes of malpractice litigation.
- Diagnostic error is implicated in 1 in 10 patient-safety incidents, costing the system an estimated CAD 3.2–3.8 billion annually in preventable expenditures. [16][17][18]
Critical Metrics and Forecast: Quantifying the Opportunity
India’s Diagnostic Burden
| Metric | Value | Source |
|---|---|---|
| Population (2024) | 1.45 billion | World Bank |
| Physician consultations per capita | ~3/year | Praxis / NITI Aayog |
| Total annual consultations | ~4.3 billion | Computed |
| Baseline diagnostic error rate | 10% | WHO / BMJ / NASEM |
| Annual diagnostic errors (2025 est.) | 43.5 crore (435 million) | Derived |
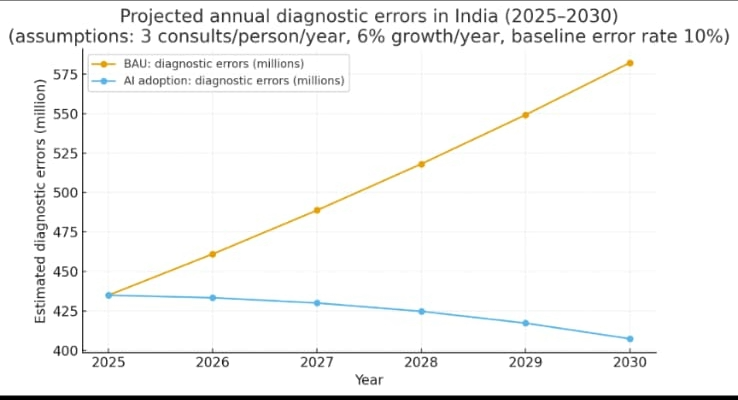
With 6% annual growth in consultations, errors will exceed 580 million by 2030 under “business as usual.” However, if AI-powered triage and support like CeaseMyPain reduce errors by even 30%, nearly 15 crore (150 million) diagnostic errors could be prevented every year. [7][8][5]
| Contributor | Share | Description |
|---|---|---|
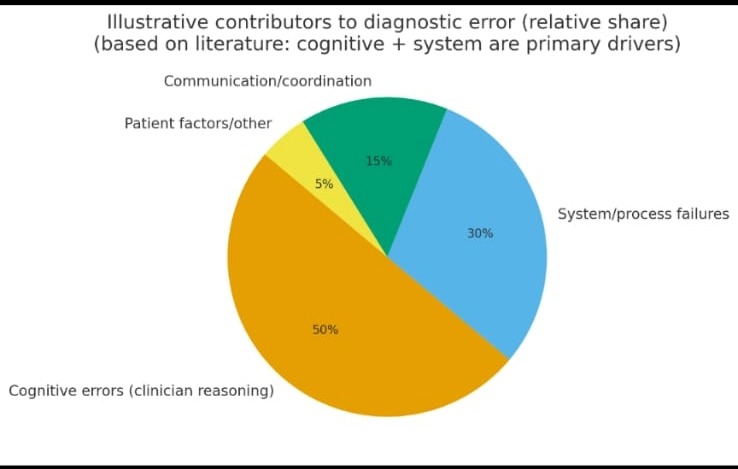
| Cognitive errors (reasoning bias) | 50–55% | Misinterpretation, premature closure |
| System/process failures | 30–35% | Fragmented records, poor follow-up |
| Communication/coordination errors | 10–15% | Handoffs, unclear instructions |
| Patient/contextual factors | 5% | Low literacy, complexity |
Cost Savings and Economic Impact
Evidence from global and Indian studies shows AI adoption drives substantial cost savings by avoiding unnecessary tests, reducing workflow errors, and preventing avoidable admissions. [9][10]
| Source | Cost Saving Metric | Estimate |
|---|---|---|
| Diagnostic test optimization | $1.01 saved per avoided test | [9] |
| Reduced workflow errors | $15.40 saved per patient annually | [10] |
| Improved outpatient efficiency | $13.20 saved per visit | [1] |
| Canadian AI pilot (CMAJ 2023) | 8–14% reduction in misdiagnosis-related claims | [18] |
Extrapolated to India:
If even 10% of India’s consultations (430 million/year) integrate AI triage:
- Potential annual direct savings: ₹9,000–11,000 crore
- Indirect savings (reduced hospitalizations, repeat tests): ₹25,000+ crore
- Lives saved or harm avoided: 1–2 million annually (based on WHO harm ratios)
Research Foundation: Mullainathan & Obermeyer (2022)
Landmark studies by Mullainathan & Obermeyer demonstrate:
- AI improves diagnostic accuracy by reducing clinician bias in identifying high-risk conditions like cardiac events and diabetes. [12][13]
- Machine-learning models significantly enhance workflow efficiency and lower costs.
- Transparent, validated models yield higher trust and better integration into real-world clinical settings.
These findings echo WHO and NASEM recommendations: AI is not to replace doctors, but to augment them.
How CeaseMyPain Directly Reduces Harm and Cost
| CeaseMyPain Feature | Diagnostic Problem Solved | System Impact |
|---|---|---|
| Structured Symptom Intake | Missed or incomplete histories | Improves data quality |
| Red-Flag Triage Detection | Delayed referrals for critical cases | Prevents severe outcomes |
| Clinical Decision Support (CDSS) | Cognitive bias, missed differentials | Enhances diagnostic accuracy |
| Continuity and Recordkeeping | Lost results, repeated tests | Reduces duplication and litigation |
| Patient Education & Tracking | Low awareness, poor follow-up | Promotes proactive care |
CeaseMyPain’s AI engine, built on validated symptom-checker logic and WHO-aligned frameworks, bridges the diagnostic gap between India’s population scale and Canada’s precision care systems, adapting to both contexts.
Implementation, Safeguards, and Alignment
- Workflow Integration: Embed CeaseMyPain insights in telemedicine and EMR interfaces.
- Validation & Transparency: Use auditable AI logic for regulatory compliance (NMC India, Health Canada).
- Data Protection: Align with India’s Digital Personal Data Protection Act (2023) and Canada’s PIPEDA.
- Education: Incorporate AI diagnostic literacy into medical curricula and CME programs.
Policy & Practice Recommendations
- Scale structured AI-powered symptom intake across primary-care and telehealth channels.
- Integrate explainable CDSS into hospital EMRs for clinician oversight.
- Close the loop on test tracking and follow-ups.
- Fund pilot projects through India’s National Health Stack and Canada Health Infoway.
- Measure outcomes with metrics: error reduction %, cost savings, harm avoided, and patient satisfaction.
Conclusion: A Shared Vision for Safer, Smarter Healthcare
India and Canada represent two ends of the same spectrum — one battling overload and access gaps, the other combating systemic inefficiencies. AI apps like CeaseMyPain can bridge both worlds — augmenting clinical judgment, cutting preventable errors, and saving billions while rebuilding trust between patients and providers.
For patients, CeaseMyPain offers more than symptom tracking; it is a pathway to empowerment and safety. For systems, it offers a blueprint for measurable efficiency gains and human impact.
References
[1] WHO – Diagnostic Errors and Patient Safety, 2023
[2] National Academies of Sciences, Improving Diagnosis in Health Care (2015)
[3] TechSci Research, AI in Medical Diagnostics Market – India (2024)
[4] Urban Institute, Building Equitable AI in Health Care (2023)
[5] Mullainathan, S. & Obermeyer, Z., The Economics of AI in Health Care (NBER, 2022)
[6] Custom Market Insights, India AI Diagnostics Report (2023)
[7] NBER, Economics of Artificial Intelligence in Health Care (2021)
[8] Healthcare Bulletin, 2024 – AI in Internal Medicine Study
[9] Cureus, Economic Evaluation of AI in Health Care (2024)
[10] IEEE Access, AI-driven Efficiency and Cost Reduction in Clinical Workflows (2024)
[11] ScienceDirect, AI Models for Diagnostic Safety (2024)
[12] NBER Working Paper c14761, Machine Learning and Health Outcomes
[13] SSRN, Clinical Validation of AI Diagnostic Models (2023)
[14] EasyClinic.io, AI in Diagnostic Accuracy (2023)
[15] Ken Research, India AI Diagnostics Market Report (2024)
[16] CMAJ, Reducing Diagnostic Error in Canada (2023)
[17] Nature Digital Medicine, AI in Canadian Health Systems (2024)
[18] PMC, Diagnostic Error and Patient Safety in Canada (2022)
[19] Nature (npj Digital Medicine), Responsible AI Adoption in Healthcare (2024)
